
Vitamin D quantities are measured in International Units (IU), with one IU being equivalent to 0.025 micrograms. One microgram is therefore 40 IU and one milligram is 40,000 IU. The research we quote can use IU and grams interchangeably.
Can you have too much vitamin D? Should you take supplements? Take a look at Adrian’s overview of the latest scientific research into vitamin D toxicity.
What is Vitamin D Good For?
Rickets used to be the scourge of children: young lives irretrievably damaged by misshapen bone growth. In the early 20th century its cause was identified as a lack of sunlight and from that came the discovery of vitamin D. With the application of the right nutrition and more sunshine, rickets was eradicated from developed economies almost overnight, one of the many triumphs of medicine of that era.
Eager to find more applications for this exciting discovery, the vitamin was very soon prescribed for many ailments and exceptionally large doses were prescribed to sufferers of rheumatoid arthritis. Quantities of Vitamin D are measured in International Units (IU), with a single IU being one fortieth (0.025%) of a microgram (µg). At that time daily prescriptions of hundreds of thousands of IU, even millions, were commonplace.
Can You Overdose on Vitamin D?
This came to a halt in the late 1940s when symptoms of hypercalcaemia – too much calcium in the blood – were diagnosed in some of those prescribed. The connection to vitamin D was obvious as its main role is to aid the body’s absorption of calcium, hence its crucial role in bone health, so an excess of calcium absorption could easily accompany an excess of vitamin D.
The phrase Vitamin D Toxicity (VDT) was coined, with hypercalcemia as its principal symptom. THis is a very serious condition manifesting in kidney stones, osteoporosis and heart disease. The response of the medical profession was draconian. Vitamin D in infants was to be monitored and, if lacking, remedied quickly and easily, with supplements if necessary, but vitamin D as a form of treatment in any other context was too risky. The mere fact of there being an upper safety limit, even if indeterminate, was sufficient to deter the medical profession from further experimentation. Public policy consolidated this ultra-cautious approach.

More recently, however, the balance between risk and remedy has tilted back in favour of the vitamin as it has been linked to areas other than infant bone growth. A correlation between depressive mood and vitamin D deficiency has been widely chronicled.
Extensive anecdotal evidence has also accumulated that links its deficiency to chronic pain.
- 2013: “Vitamin D and chronic pain in the elderly”
- 2015: “Is Serum Hypovitaminosis D Associated with Chronic Widespread Pain Including Fibromyalgia? A Meta-analysis of Observational Studies”
- 2016: “Vitamin D for the treatment of painful diabetic neuropathy”
Furthermore, as lives in developed economies became ever more sedentary and indoors, a deficiency in the vitamin has become a matter of serious social concern. Clearly the problem is not limited to infants and it has become important – even urgent – to establish its optimal level in adult bodies. How much is enough and how much is too much?
When to Take Vitamin D
The standard vitamin D blood test measures the concentration of 25-hydroxy (OH) vitamin D (one of its many derivatives) in the blood, so called “serum concentration”. The unit is in nanograms per millilitre (ng/ml). A reading below 20 indicates a severe deficiency but when it comes to an optimal or maximum level, there is no consensus. These are the levels recommended by various bodies.
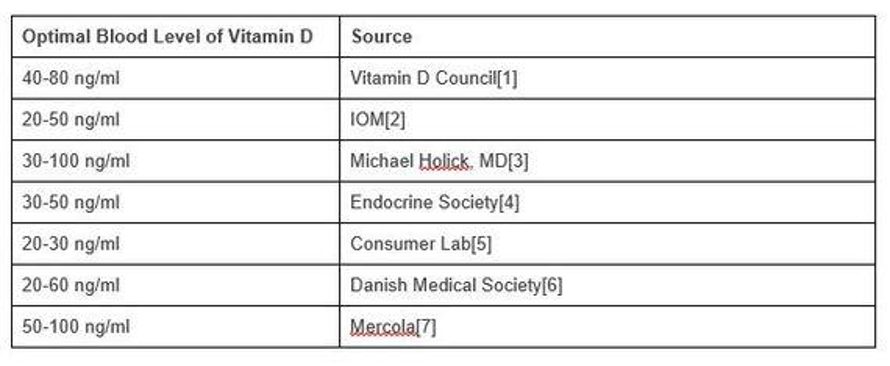
Source: https://www.huffpost.com/entry/update-how-much-vitamin-d_b_11254120
On the one hand, anywhere between 30 and 100 may be optimal. On the other hand, anything above 30 might be excessive. Unhelpful.
In my own personal experience, I had a reading of 20 ng/ml and my doctor recommended I get that up to 80 ng/ml. On balance, it seems, the profession has inverted its previous stance and is now biased towards higher levels.
But let’s say one does establish an optimum, say 80 ng/ml – how much supplement do I need to take to obtain this level? There is no easy answer to that either.
[16] Heaney RP, et al., “25-Hydroxylation of vitamin D3: relation to circulating vitamin D3 under varying input conditions,” American Journal of Clinical Nutrition, 87: 1730-1737, 2008. Source: https://www.huffpost.com/entry/update-how-much-vitamin-d_b_11254120
This chart shows the serum concentrations of patients taking differing daily dosages and what it illustrates is that there is virtually no relationship between your serum concentration and your supplement intake. Even up to 20,000 IU daily your serum levels may not achieve my recommended 80ng/ml; or you could be taking no supplement at all and find your level above 100 ng/ml.
Such imprecise outcomes have not been helpful in persuading policymakers to relax their fearful grip on recommended daily allowances. Definitive answers have been even harder to come by because the chemistry of Vitamin D is too complex:
- 2010: “Vitamin D Metabolism”
- 2010: “‘Pharmacokinetics of vitamin D toxicity.’ The most thorough explanation of how VDT gives rise to hypercalcemia”
But this is also because each of our responses is too individualistic for strong generalisations to be made.
Medical Opinions on the Correct Dosage
The medical profession has nevertheless been willing to push the boundaries towards higher doses as they can see at first hand the health benefits. Following my own diagnosis, I was prescribed a weekly loading dose of 50,000 IU and a daily maintenance dose of 4,000 IU. It’s a hefty bump but will it be enough? I won’t know without trying.
One reason to be bold is because oral dosage is not our main source of the vitamin. We manufacture very large quantities simply by standing in sunlight and about this we know two things: we can always obtain sufficient vitamin D in this manner and we will never be at risk of VDT. Whatever quantities we make from sunlight must be inherently safe.
How much can we make? The general consensus is:



